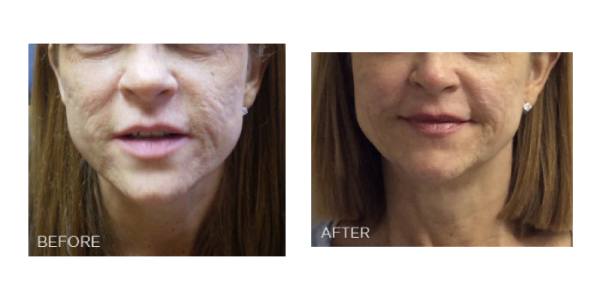
Types of Acne Scars
ICE-PICK SCARS
Typically deep pits that can occur anywhere on the face.
SHALLOW, DEPRESSED SCARS
Typically slightly depressed areas, which can often look like shallow chickenpox scars
DEEPER, DEPRESSED SCARS
Deeper depressions which occurs most commonly on the cheeks
For many patients, there is no one procedure that will accomplish all of one’s goals. Therefore, is often best to use a combined approach utilizing two or more different procedures to achieve an optimal result. Occasionally these procedures can be performed at the same time, although often these procedures are performed several weeks apart. Below is a list of commonly performed procedures, their limitations and benefits.

Treatment modalities commonly used for shallow, depressed scars
Laser-Peel (carbon dioxide or Erbium:YAG):
Unlike chemical peels which rely on acids to damage the skin, the laser-peel utilizes laser energy to precisely peel away layers of skin. This type of peel works best for depressed scars. Like the medium-depth chemical peel, recovery typically takes several weeks and redness can persist for months. Additionally, redness of the treated area may last for several months. The final result may not be fully appreciated for one year or longer. Fractional CO2 Laser Resurfacing is an improved version of the traditional ablative CO2 laser, and has faster healing than traditional ablative CO2 laser resurfacing.
Dermabrasion:
With this modality, layers of skin are sanded away. In general, dermabrasion typically works best for shallow depressed scars, with only modest improvement, if any, on ice-pick scars. The recovery or dermabrasion typically is one or more weeks, although redness of the skin can persist for several months.
Microneedling with radiofrequency (i.e. Secret RF):
Electrical energy, radiofrequency, is used to tighten the skin. The tiny microneedles are used to deliver the energy. It is the radiofrequency that results in tightening of the skin and reduction of the scars. Results are often impressive, although multiple treatments are often needed.
Restylane™ or Juvederm™ Injections:
This product is injected directly into the scar. There is little to no recovery in most cases. Unfortunately, results are not permanent, but often last six months or longer.
Fraxel™ Erbium Laser:
This laser ablates tiny spots of tissue. Unlike tradition Laser-peeling, several treatment sessions are needed and mild-moderate improvement can be achieved. The advantage of this modality over traditional Carbon Dioxide Laser-Peels is that healing is fast (days), but the results with a single treatment is not as good.
Superficial Chemical Peel (glycolic acid, salicylic acid peels, and 15-20% TCA):
These superficial peels are often used to improve very mild acne and/or staining of the skin (dark spots). In general, these peels affect mainly the epidermis (the top layer of skin). Unfortunately, the superficial peels offer little improvement with acne scars, where the damage is in deeper layers of the skin–the dermis. In general, these peels offer little or no improvement of ice-pick scars, and minimal improvement of shallow depressed scars. One of the benefits of these superficial peels is that there is minimal recovery needed. Most patients will experience some peeling, redness, and/or flaking of the skin for up to week.
Microneedling:
Tiny needles are rolled or inserted into the skin. This minor injury results in the release of proteins that result in slight improvement of scars. Multiple treatments are needed and results are often unimpressive.
Medium-Depth Chemical Peel (70% glycolic acid or 35%+TCA peels):
These peels are often used to improve wrinkles or superficial scars, including acne scars. Depending upon the depth of peel achieved, recovery may be several days to several weeks or longer. This type of peel works best for shallow depressed scars, with minimal affect on ice-pick scars.
Treatment modalities commonly used for deeper, depressed scars
Subcision with Dermal Filler:
For scars that are tethered (pulled down with scar tissue), the release of these tethers is paramount in order to get the skin to come back up. A special needle is used to cut the tethers and a dermal filler (Restylane™ or Juvederm™) is then placed to reduce the chance of the tethers reforming. The fillers are not permanent and may need to be replaced every 6-12 months.
Radiesse™:
This product is injected under the scar to create immediate elevation. Results last 6-18 months typically. Results are usually predictably good to excellent.
Fat Transplantation:
In this procedure, fat is taken from one area of the body (usually the hip) and mesh transplanted beneath the depressed scar to elevate it. Occasionally, multiple procedures may be necessary to achieve optimal results. Results may or may not be permanent. Patients are usually required to abstain from any exertional activity for one week or longer after the procedure. Additionally, some mild swelling may result in the procedure, although typically resolve within several days.
Gore-tex™ Implantation:
Gore-tex, which is commonly used in clothing, is made into strands, threads, and mesh-like material. This material is placed directly beneath the depressed scars, thus elevating them. Correction using Gore-tex may be permanent, although the implant material can be felt under the skin. This procedure requires little or no recovery time. This is not commonly performed.
Excision:
Deeper scars may be cut out using a scalpel and stitched together. This results in the formation of a linear scar, which in some cases may look better than the depressed scar.
Punch Grafting:
With this procedure, small depressed scars are cut out using a small “punch”, which resembles a small cookie cutter. A small piece of skin is then removed, using a “punch”, from in front of or behind the ear and transplanted to where the scar was located. This new transplant skin is then secured in place using special tape strips or glue. The hole from where the skin was removed from in front of or behind-the ear is sutured using stitches. Often, several weeks later a dermabrasion or laser-peel is performed.
Sculptra™:
This product is injected under the scar. Most patients have 2-3 treatments spaced 6 weeks apart. Results are somewhat less predictable than other methods, such as Radiesse™, but can last for years.
Artefill™:
This product contains tiny Plexiglass™ beads that are injected under the scar, creating a permanent result. Reactions are possible to the material that can result in prolonged redness, although this is uncommon.
Silicone:
This product is not FDA approved for cosmetic purposes, but has been used for decades. Results are permanent, but must be used with caution and in experienced hands.
Treatment modalities commonly used for the treatment of ice-pick scars
Cross TCA:
80 – 100% trichloroacetic acid (TCA) is put directly into the scar to shrink them. This procedure is simple, takes minutes, and results in small crusts at the treated scar. More than one treatment is usually needed, but the results are often substantial.
Punch Grafting:
With this procedure, small depressed scars are cut out using a small “punch”, which resembles a small cookie cutter. A small piece of skin is then removed, using a “punch”, from in-front-of or behind-the ear and transplanted to where the scar was located. This new transplant skin is then secured in place using special tape strips or glue. The hole from where the skin was removed from in-front-of or behind-the ear is sutured using stitches. Often, several weeks later a dermabrasion or laser-peel is performed.
Excision:
Deeper scars, including ice-pick scars, may be cut out using a scalpel and stitched together. This results in the formation of a linear scar.
Laser-Peel (carbon dioxide or Erbium:YAG): more recently, the laser-peel has been used for ice-pick scars. Unfortunately, results are typically inferior to other methods such as punch grafting or excision unless combined with excision or punch grafting.
Summary
As with most cosmetic surgery, treatment options must be considered on individual basis, as no one procedure is best for all. In many cases, one procedure may not afford as much benefit as two or more procedures. Therefore it is essential to evaluate each person on individual basis and devise a treatment plan based on the patient’s desires for improvement, recovery time needed, cost, and the risks of the procedure(s).
Treatment modalities commonly used for shallow, depressed scars
Fraxel™ Erbium Laser:
This laser ablates tiny spots of tissue. Unlike tradition Laser-peeling, several treatment sessions are needed and mild-moderate improvement can be achieved. The advantage of this modality over traditional Carbon Dioxide Laser-Peels is that healing is fast (days), but the results with a single treatment is not as good.
Superficial Chemical Peel (glycolic acid, salicylic acid peels, and 15-20% TCA):
These superficial peels are often used to improve very mild acne and/or staining of the skin (dark spots). In general, these peels affect mainly the epidermis (the top layer of skin). Unfortunately, the superficial peels offer little improvement with acne scars, where the damage is in deeper layers of the skin–the dermis. In general, these peels offer little or no improvement of ice-pick scars, and minimal improvement of shallow depressed scars. One of the benefits of these superficial peels is that there is minimal recovery needed. Most patients will experience some peeling, redness, and/or flaking of the skin for up to week.
Microneedling:
Tiny needles are rolled or inserted into the skin. This minor injury results in the release of proteins that result in slight improvement of scars. Multiple treatments are needed and results are often unimpressive.
Medium-Depth Chemical Peel (70% glycolic acid or 35%+TCA peels):
These peels are often used to improve wrinkles or superficial scars, including acne scars. Depending upon the depth of peel achieved, recovery may be several days to several weeks or longer. This type of peel works best for shallow depressed scars, with minimal affect on ice-pick scars.
What is Botox® ?
Botox® is a toxin (toxic substance) which is naturally produced by the bacteria called Clostridium botulinum. Interestingly, it is currently believed to be the most toxic poison known to man, although the use of such tiny amounts has been used safely in man for over twenty-five years. This bacteria produces several types of toxin, of which only “type A” is used for medicinal purposes today.
How does Botox® work?
The Botox® toxin works where the nerve meets the muscle where the nerve sends its signal telling the muscle to contract. This results in paralysis of the treated muscle.
How long does a Botox® treatment result last?
Unfortunately, Botox® results are not permanent. Initial treatments for wrinkles typically last 3 to 4 months. Subsequent treatments may prove to have more lasting results. Treatment of hyperhidrosis (excessive sweating) may last up to one year (average 5.2 months)
What wrinkles can be treated using Botox® ?
Although Botox® is only FDA approved for treatment of the frown lines (glabella), Botox® has been used with good to excellent results for the treatment of the forehead wrinkles and crow’s feet. Infraorbital wrinkles (wrinkles below the eyes) can be treated with moderate results. Newer therapeutic uses have been for the treatment of nasolabial folds (smile lines), perioral wrinkles (wrinkles around the mouth), corners of the mouth, and anterior neck which carry a higher risk of complications and have mixed results.
Can Botox®treat excessive sweating (hyperhidrosis)?
Yes. Botox® has been recently FDA approved to treat hyperhidrosis of the hands and axilla (underarms) since at least 1995 with good results which may last up to 12 months (average 5.2 months). Treatment of the hands has resulted in mild weakness of the hands in a few patients as a result of toxin diffusion to the intrinsic muscles of the hand (muscles within the hand). Since this finding, more superficial injections have been used with good success and a lower incidence of weakness.
Who should not get treated with Botox®?
Botox® has not been studied in pregnancy, and it is therefore unknown if fetal harm will result if a pregnant woman is treated with Botox®. Therefore, the use of Botox® is not recommended during pregnancy. Additionally, it is unknown if Botox® (botulinum A exotoxin) is excreted in breast milk, where it could affect a nursing infant. Therefore, Botox® treatment is not recommended for use in lactating women. Additionally, patients with neuromuscular disease, such as myasthenia gravis and Eaton-Lambert syndrome, should not be treated with Botox® as it may worsen these conditions. Of course, anyone who has had an allergic reaction to Botox® should not be treated.
What are the side effects and complications (problems) associated with treatments with Botox® ?
As Botox® is injected directly into the muscle body when used for wrinkles, bruising may occur. This can be minimized if patients avoid the use of aspirin, aspirin-containing products, and non-steroidal anti-inflammatory agents (i.e. ibuprofen, Motrin® , Advil® , naproxen, Aleve) for one week before treatment, although this is not necessary. Rarely, generalized reactions have been reported include nausea, fatigue, malaise, skin rash, and flu-like symptoms. It has been postulated that these generalized reactions occur from diffusion of minute amounts of the toxin into the circulatory system of which the significance of such reaction is unknown.
With treatment of the glabella (frown lines), ptosis (drooping of the eyelid) has occurred and may persist for up to 4 weeks. Some physicians believe that if patients remain in an upright position, avoid manipulation of the area treated, and actively contract the muscles treated for 4 hours after treatment, the likelihood of ptosis (drooping) is minimized due to increased uptake of the toxin. To avoid this problem, physicians are using more concentrated toxin that results in far less diffusion (spread) of the toxin to unwanted areas and therefore even less chance of eyelid droop (ptosis). In addition, most cosmetic surgeons believe that injections over the pupil should be at least 1 cm above the eyebrow. Although ptosis is now rarely seen, it is easily treated using alpha-adrenergic agonists (mild stimulants) topically applied to the eye (eyedrops).
Occasionally the glabella (frown lines) does not respond as well as one would like (i.e. frowning still occurs), especially in men. Therefore, this area may require a second treatment in 10-14 days.
Treatment of the forehead results in a more youthful appearance (due to decreased furrows), although there is decreased expressivity. Treatment must be carefully individualized to each patient. Patients who have a low brow and/or hooding of the upper eyelid (drooping upper eyelid skin) may have a total inability to raise any part of the eyebrow and may result in brow ptosis, worsening the appearance of the eyes. This can result in decreased visual acuity and the feeling of a ‘heavy brow’. Unfortunately, there is no treatment for this if it occurs, although the effects will wear off within 3-4 months. To avoid this, most cosmetic surgeons believe that treatment of the forehead should be above the first forehead wrinkle or at least 1-cm above the eyebrow. This may allow for some movement of the eyebrow. When the lateral fibers of the frontalis muscle (forehead muscles which wrinkle the forehead) have not been adequately paralyzed, a quizzical appearance may result in which one or both of the lateral eyebrows can be raised while the central portions remains depressed. This can be easily remedied by treating the lateral frontalis muscle (forehead muscles which wrinkle the forehead).
Bruising often follows treatment of the crow’s feet, occurs occasionally with treatment of the forehead, and rarely with treatment of the frown lines. Drooping of the lower lid margin and double vision have been reported, which can be avoided by injecting the toxin at least 1 cm from the lateral canthus (corner of the eye).
Treatment of the platysma (neck bands) has been reported to result in dysphagia (difficulty swallowing). Treatment with meloclopramide (Reglan) may improve swallowing if this occurs.
Treatment of the palms for hyperhidrosis (excessive sweating) has been reported to result in slight hand weakness in some patients. It is presumed that this has occurred due to diffusion of the toxin to the intrinsic muscles in the hand (muscles within the hand). Injecting the toxin very superficially has minimized this complication.
Therapeutic failures (patients do not respond to treatment) have now been reported. It is believed that these failures result when the body makes antibodies against the toxin, therefore neutralizing it. It is believed that with cumulative doses exceeding 200-300 Units, there is an increased likelihood of developing neutralizing antibodies. Therefore, when treating hyperhidrosis or larger muscle groups, it is recommended that injections be spaced at least 1-month apart. In the future, different types of this toxin may become available for clinical use that may be useful for those who have developed neutralizing antibodies.
Although Botox® is often used to treat migraine headaches, there have been a few reports of recurrent headaches occurring in patients undergoing treatment with Botox® for cosmetic purposes.
History of Botox® use:
In the early 1970’s, Dr. Alan Scott began investigating the use of botulinum A exotoxin for the treatment of strabismus (crossed-eyes) in monkeys. In 1977 clinical studies were initiated in humans for the treatment of strabismus. In the mid-1980’s Dr. Scott indicated that he had treated a patient for “cosmetic reasons” using botulinum A exotoxin.
Shortly thereafter, a patient of Dr. Jean Carruthers, an ophthalmologist in Vancouver, Canada, had noticed improvement of the glabella (frown lines) after a patient was treated for blepharospasm (twitching of the eye). This finding prompted Dr. Jean Carruthers, with Dr. Alastair Carruthers, a dermatologist also practicing in Vancouver, Canada, to begin the use of botulinum A exotoxin (Botox®) for the treatment of the glabella (frown lines) and, shortly thereafter, the treatment of the crow’s feet. These results were soon published in the Journal of Dermatologic Surgery and Oncology in 1990 and presented at the annual meeting of the American Society for Dermatologic Surgery in March 1991.
These initial works inspired many dermatologic surgeons to use botulinum A exotoxin (Botox® , Dysport®) for the treatment of the glabella (frown lines), crow’s feet, and forehead which was soon followed by other specialties including plastic surgery and ophthalmology. The addition of the carbon dioxide laser to the cosmetic surgeon’s armamentarium has resulted in a resurgence in the cosmetic surgery field. Dr. David Duffy in one of the pioneers who began using botulinum toxin with laser resurfacing which was reported by the Carruthers in Dermatologic Surgery in 1998. Soon thereafter, trials were begun using botulinum A exotoxin in combination with other cosmetic procedures including endoscopic brow lift, upper and lower blepharoplasty (eyelid surgery), and in the lower face with facelifting. Platysmal bands, which are found in the front of the neck, were found to be responsive to treatment with botulinum A exotoxin by Blitzer et al. The treatment of axillary hyperhidrosis (excessive sweating under the arms) and palmar hyperhidrosis (excessive sweating of the hands) was introduced in 1995 by Bushara et al. with moderate success.
Now, more than twenty-five years after Dr. Alan Scott first described the clinical use of botulinum A exotoxin (Botox®) for the treatment of strabismus (crossed-eyes), the clinical possibilities for botulinum A exotoxin is most limited by our imagination.
How long does the treatment take?
Most treatments can be accomplished within 10-15 minutes–one of the so-called “lunch-time” procedures. Most patients will have no evidence of having anything done, although some will have mild bruising (particularly when treating the Crow’s feet).
Do I need to take off from work or other activities?
For 3-4 hours after the procedure it is recommended that the patient remain in the upright position. Additionally, it is best to avoid strenuous or jarring activities such as exercising, running, or jogging for at least 3-4 hours. Nearly all patients may return to work immediately following the procedure and resume exercise the following day?
Do the treatments hurt?
The treatments consist of a series of tiny injections using a fine needle. Although most patients tolerate the treatments with little discomfort, some patients request the use of a topical anesthetic which is applied to the areas to be treated 1-2 hours before the scheduled appointment.
How much does Botox® treatments cost?
The toxin itself is expensive. The cost varies from doctor to doctor, and depends on which area(s) are to be treated. Some doctors charge according to the amount of toxin used while others charge per “zone” treated. The average cost per “zone” is approximately $260.00 – $500.00. A “zone” would be any one of the following: glabella (frown lines), forehead, or crow’s feet.
What is Botox® ?
Botox® is a toxin (toxic substance) which is naturally produced by the bacteria called Clostridium botulinum. Interestingly, it is currently believed to be the most toxic poison known to man, although the use of such tiny amounts has been used safely in man for over twenty-five years. This bacteria produces several types of toxin, of which only “type A” is used for medicinal purposes today.
How does Botox® work?
The Botox® toxin works where the nerve meets the muscle where the nerve sends its signal telling the muscle to contract. This results in paralysis of the treated muscle.
How long does a Botox® treatment result last?
Unfortunately, Botox® results are not permanent. Initial treatments for wrinkles typically last 3 to 4 months. Subsequent treatments may prove to have more lasting results. Treatment of hyperhidrosis (excessive sweating) may last up to one year (average 5.2 months)
What wrinkles can be treated using Botox® ?
Although Botox® is only FDA approved for treatment of the frown lines (glabella), Botox® has been used with good to excellent results for the treatment of the forehead wrinkles and crow’s feet. Infraorbital wrinkles (wrinkles below the eyes) can be treated with moderate results. Newer therapeutic uses have been for the treatment of nasolabial folds (smile lines), perioral wrinkles (wrinkles around the mouth), corners of the mouth, and anterior neck which carry a higher risk of complications and have mixed results.
Can Botox®treat excessive sweating (hyperhidrosis)?
Yes. Botox® has been recently FDA approved to treat hyperhidrosis of the hands and axilla (underarms) since at least 1995 with good results which may last up to 12 months (average 5.2 months). Treatment of the hands has resulted in mild weakness of the hands in a few patients as a result of toxin diffusion to the intrinsic muscles of the hand (muscles within the hand). Since this finding, more superficial injections have been used with good success and a lower incidence of weakness.
Who should not get treated with Botox®?
Botox® has not been studied in pregnancy, and it is therefore unknown if fetal harm will result if a pregnant woman is treated with Botox®. Therefore, the use of Botox® is not recommended during pregnancy. Additionally, it is unknown if Botox® (botulinum A exotoxin) is excreted in breast milk, where it could affect a nursing infant. Therefore, Botox® treatment is not recommended for use in lactating women. Additionally, patients with neuromuscular disease, such as myasthenia gravis and Eaton-Lambert syndrome, should not be treated with Botox® as it may worsen these conditions. Of course, anyone who has had an allergic reaction to Botox® should not be treated.
What are the side effects and complications (problems) associated with treatments with Botox® ?
As Botox® is injected directly into the muscle body when used for wrinkles, bruising may occur. This can be minimized if patients avoid the use of aspirin, aspirin-containing products, and non-steroidal anti-inflammatory agents (i.e. ibuprofen, Motrin® , Advil® , naproxen, Aleve) for one week before treatment, although this is not necessary. Rarely, generalized reactions have been reported include nausea, fatigue, malaise, skin rash, and flu-like symptoms. It has been postulated that these generalized reactions occur from diffusion of minute amounts of the toxin into the circulatory system of which the significance of such reaction is unknown.
With treatment of the glabella (frown lines), ptosis (drooping of the eyelid) has occurred and may persist for up to 4 weeks. Some physicians believe that if patients remain in an upright position, avoid manipulation of the area treated, and actively contract the muscles treated for 4 hours after treatment, the likelihood of ptosis (drooping) is minimized due to increased uptake of the toxin. To avoid this problem, physicians are using more concentrated toxin that results in far less diffusion (spread) of the toxin to unwanted areas and therefore even less chance of eyelid droop (ptosis). In addition, most cosmetic surgeons believe that injections over the pupil should be at least 1 cm above the eyebrow. Although ptosis is now rarely seen, it is easily treated using alpha-adrenergic agonists (mild stimulants) topically applied to the eye (eyedrops).
Occasionally the glabella (frown lines) does not respond as well as one would like (i.e. frowning still occurs), especially in men. Therefore, this area may require a second treatment in 10-14 days.
Treatment of the forehead results in a more youthful appearance (due to decreased furrows), although there is decreased expressivity. Treatment must be carefully individualized to each patient. Patients who have a low brow and/or hooding of the upper eyelid (drooping upper eyelid skin) may have a total inability to raise any part of the eyebrow and may result in brow ptosis, worsening the appearance of the eyes. This can result in decreased visual acuity and the feeling of a ‘heavy brow’. Unfortunately, there is no treatment for this if it occurs, although the effects will wear off within 3-4 months. To avoid this, most cosmetic surgeons believe that treatment of the forehead should be above the first forehead wrinkle or at least 1-cm above the eyebrow. This may allow for some movement of the eyebrow. When the lateral fibers of the frontalis muscle (forehead muscles which wrinkle the forehead) have not been adequately paralyzed, a quizzical appearance may result in which one or both of the lateral eyebrows can be raised while the central portions remains depressed. This can be easily remedied by treating the lateral frontalis muscle (forehead muscles which wrinkle the forehead).
Bruising often follows treatment of the crow’s feet, occurs occasionally with treatment of the forehead, and rarely with treatment of the frown lines. Drooping of the lower lid margin and double vision have been reported, which can be avoided by injecting the toxin at least 1 cm from the lateral canthus (corner of the eye).
Treatment of the platysma (neck bands) has been reported to result in dysphagia (difficulty swallowing). Treatment with meloclopramide (Reglan) may improve swallowing if this occurs.
Treatment of the palms for hyperhidrosis (excessive sweating) has been reported to result in slight hand weakness in some patients. It is presumed that this has occurred due to diffusion of the toxin to the intrinsic muscles in the hand (muscles within the hand). Injecting the toxin very superficially has minimized this complication.
Therapeutic failures (patients do not respond to treatment) have now been reported. It is believed that these failures result when the body makes antibodies against the toxin, therefore neutralizing it. It is believed that with cumulative doses exceeding 200-300 Units, there is an increased likelihood of developing neutralizing antibodies. Therefore, when treating hyperhidrosis or larger muscle groups, it is recommended that injections be spaced at least 1-month apart. In the future, different types of this toxin may become available for clinical use that may be useful for those who have developed neutralizing antibodies.
Although Botox® is often used to treat migraine headaches, there have been a few reports of recurrent headaches occurring in patients undergoing treatment with Botox® for cosmetic purposes.
History of Botox® use:
In the early 1970’s, Dr. Alan Scott began investigating the use of botulinum A exotoxin for the treatment of strabismus (crossed-eyes) in monkeys. In 1977 clinical studies were initiated in humans for the treatment of strabismus. In the mid-1980’s Dr. Scott indicated that he had treated a patient for “cosmetic reasons” using botulinum A exotoxin.
Shortly thereafter, a patient of Dr. Jean Carruthers, an ophthalmologist in Vancouver, Canada, had noticed improvement of the glabella (frown lines) after a patient was treated for blepharospasm (twitching of the eye). This finding prompted Dr. Jean Carruthers, with Dr. Alastair Carruthers, a dermatologist also practicing in Vancouver, Canada, to begin the use of botulinum A exotoxin (Botox®) for the treatment of the glabella (frown lines) and, shortly thereafter, the treatment of the crow’s feet. These results were soon published in the Journal of Dermatologic Surgery and Oncology in 1990 and presented at the annual meeting of the American Society for Dermatologic Surgery in March 1991.
These initial works inspired many dermatologic surgeons to use botulinum A exotoxin (Botox® , Dysport®) for the treatment of the glabella (frown lines), crow’s feet, and forehead which was soon followed by other specialties including plastic surgery and ophthalmology. The addition of the carbon dioxide laser to the cosmetic surgeon’s armamentarium has resulted in a resurgence in the cosmetic surgery field. Dr. David Duffy in one of the pioneers who began using botulinum toxin with laser resurfacing which was reported by the Carruthers in Dermatologic Surgery in 1998. Soon thereafter, trials were begun using botulinum A exotoxin in combination with other cosmetic procedures including endoscopic brow lift, upper and lower blepharoplasty (eyelid surgery), and in the lower face with facelifting. Platysmal bands, which are found in the front of the neck, were found to be responsive to treatment with botulinum A exotoxin by Blitzer et al. The treatment of axillary hyperhidrosis (excessive sweating under the arms) and palmar hyperhidrosis (excessive sweating of the hands) was introduced in 1995 by Bushara et al. with moderate success.
Now, more than twenty-five years after Dr. Alan Scott first described the clinical use of botulinum A exotoxin (Botox®) for the treatment of strabismus (crossed-eyes), the clinical possibilities for botulinum A exotoxin is most limited by our imagination.
How long does the treatment take?
Most treatments can be accomplished within 10-15 minutes–one of the so-called “lunch-time” procedures. Most patients will have no evidence of having anything done, although some will have mild bruising (particularly when treating the Crow’s feet).
Do I need to take off from work or other activities?
For 3-4 hours after the procedure it is recommended that the patient remain in the upright position. Additionally, it is best to avoid strenuous or jarring activities such as exercising, running, or jogging for at least 3-4 hours. Nearly all patients may return to work immediately following the procedure and resume exercise the following day?
Do the treatments hurt?
The treatments consist of a series of tiny injections using a fine needle. Although most patients tolerate the treatments with little discomfort, some patients request the use of a topical anesthetic which is applied to the areas to be treated 1-2 hours before the scheduled appointment.
How much does Botox® treatments cost?
The toxin itself is expensive. The cost varies from doctor to doctor, and depends on which area(s) are to be treated. Some doctors charge according to the amount of toxin used while others charge per “zone” treated. The average cost per “zone” is approximately $260.00 – $500.00. A “zone” would be any one of the following: glabella (frown lines), forehead, or crow’s feet.
What is Botox® ?
Botox® is a toxin (toxic substance) which is naturally produced by the bacteria called Clostridium botulinum. Interestingly, it is currently believed to be the most toxic poison known to man, although the use of such tiny amounts has been used safely in man for over twenty-five years. This bacteria produces several types of toxin, of which only “type A” is used for medicinal purposes today.
How does Botox® work?
The Botox® toxin works where the nerve meets the muscle where the nerve sends its signal telling the muscle to contract. This results in paralysis of the treated muscle.
How long does a Botox® treatment result last?
Unfortunately, Botox® results are not permanent. Initial treatments for wrinkles typically last 3 to 4 months. Subsequent treatments may prove to have more lasting results. Treatment of hyperhidrosis (excessive sweating) may last up to one year (average 5.2 months)
What wrinkles can be treated using Botox® ?
Although Botox® is only FDA approved for treatment of the frown lines (glabella), Botox® has been used with good to excellent results for the treatment of the forehead wrinkles and crow’s feet. Infraorbital wrinkles (wrinkles below the eyes) can be treated with moderate results. Newer therapeutic uses have been for the treatment of nasolabial folds (smile lines), perioral wrinkles (wrinkles around the mouth), corners of the mouth, and anterior neck which carry a higher risk of complications and have mixed results.
Can Botox®treat excessive sweating (hyperhidrosis)?
Yes. Botox® has been recently FDA approved to treat hyperhidrosis of the hands and axilla (underarms) since at least 1995 with good results which may last up to 12 months (average 5.2 months). Treatment of the hands has resulted in mild weakness of the hands in a few patients as a result of toxin diffusion to the intrinsic muscles of the hand (muscles within the hand). Since this finding, more superficial injections have been used with good success and a lower incidence of weakness.
Who should not get treated with Botox®?
Botox® has not been studied in pregnancy, and it is therefore unknown if fetal harm will result if a pregnant woman is treated with Botox®. Therefore, the use of Botox® is not recommended during pregnancy. Additionally, it is unknown if Botox® (botulinum A exotoxin) is excreted in breast milk, where it could affect a nursing infant. Therefore, Botox® treatment is not recommended for use in lactating women. Additionally, patients with neuromuscular disease, such as myasthenia gravis and Eaton-Lambert syndrome, should not be treated with Botox® as it may worsen these conditions. Of course, anyone who has had an allergic reaction to Botox® should not be treated.
What are the side effects and complications (problems) associated with treatments with Botox® ?
As Botox® is injected directly into the muscle body when used for wrinkles, bruising may occur. This can be minimized if patients avoid the use of aspirin, aspirin-containing products, and non-steroidal anti-inflammatory agents (i.e. ibuprofen, Motrin® , Advil® , naproxen, Aleve) for one week before treatment, although this is not necessary. Rarely, generalized reactions have been reported include nausea, fatigue, malaise, skin rash, and flu-like symptoms. It has been postulated that these generalized reactions occur from diffusion of minute amounts of the toxin into the circulatory system of which the significance of such reaction is unknown.
With treatment of the glabella (frown lines), ptosis (drooping of the eyelid) has occurred and may persist for up to 4 weeks. Some physicians believe that if patients remain in an upright position, avoid manipulation of the area treated, and actively contract the muscles treated for 4 hours after treatment, the likelihood of ptosis (drooping) is minimized due to increased uptake of the toxin. To avoid this problem, physicians are using more concentrated toxin that results in far less diffusion (spread) of the toxin to unwanted areas and therefore even less chance of eyelid droop (ptosis). In addition, most cosmetic surgeons believe that injections over the pupil should be at least 1 cm above the eyebrow. Although ptosis is now rarely seen, it is easily treated using alpha-adrenergic agonists (mild stimulants) topically applied to the eye (eyedrops).
Occasionally the glabella (frown lines) does not respond as well as one would like (i.e. frowning still occurs), especially in men. Therefore, this area may require a second treatment in 10-14 days.
Treatment of the forehead results in a more youthful appearance (due to decreased furrows), although there is decreased expressivity. Treatment must be carefully individualized to each patient. Patients who have a low brow and/or hooding of the upper eyelid (drooping upper eyelid skin) may have a total inability to raise any part of the eyebrow and may result in brow ptosis, worsening the appearance of the eyes. This can result in decreased visual acuity and the feeling of a ‘heavy brow’. Unfortunately, there is no treatment for this if it occurs, although the effects will wear off within 3-4 months. To avoid this, most cosmetic surgeons believe that treatment of the forehead should be above the first forehead wrinkle or at least 1-cm above the eyebrow. This may allow for some movement of the eyebrow. When the lateral fibers of the frontalis muscle (forehead muscles which wrinkle the forehead) have not been adequately paralyzed, a quizzical appearance may result in which one or both of the lateral eyebrows can be raised while the central portions remains depressed. This can be easily remedied by treating the lateral frontalis muscle (forehead muscles which wrinkle the forehead).
Bruising often follows treatment of the crow’s feet, occurs occasionally with treatment of the forehead, and rarely with treatment of the frown lines. Drooping of the lower lid margin and double vision have been reported, which can be avoided by injecting the toxin at least 1 cm from the lateral canthus (corner of the eye).
Treatment of the platysma (neck bands) has been reported to result in dysphagia (difficulty swallowing). Treatment with meloclopramide (Reglan) may improve swallowing if this occurs.
Treatment of the palms for hyperhidrosis (excessive sweating) has been reported to result in slight hand weakness in some patients. It is presumed that this has occurred due to diffusion of the toxin to the intrinsic muscles in the hand (muscles within the hand). Injecting the toxin very superficially has minimized this complication.
Therapeutic failures (patients do not respond to treatment) have now been reported. It is believed that these failures result when the body makes antibodies against the toxin, therefore neutralizing it. It is believed that with cumulative doses exceeding 200-300 Units, there is an increased likelihood of developing neutralizing antibodies. Therefore, when treating hyperhidrosis or larger muscle groups, it is recommended that injections be spaced at least 1-month apart. In the future, different types of this toxin may become available for clinical use that may be useful for those who have developed neutralizing antibodies.
Although Botox® is often used to treat migraine headaches, there have been a few reports of recurrent headaches occurring in patients undergoing treatment with Botox® for cosmetic purposes.
History of Botox® use:
In the early 1970’s, Dr. Alan Scott began investigating the use of botulinum A exotoxin for the treatment of strabismus (crossed-eyes) in monkeys. In 1977 clinical studies were initiated in humans for the treatment of strabismus. In the mid-1980’s Dr. Scott indicated that he had treated a patient for “cosmetic reasons” using botulinum A exotoxin.
Shortly thereafter, a patient of Dr. Jean Carruthers, an ophthalmologist in Vancouver, Canada, had noticed improvement of the glabella (frown lines) after a patient was treated for blepharospasm (twitching of the eye). This finding prompted Dr. Jean Carruthers, with Dr. Alastair Carruthers, a dermatologist also practicing in Vancouver, Canada, to begin the use of botulinum A exotoxin (Botox®) for the treatment of the glabella (frown lines) and, shortly thereafter, the treatment of the crow’s feet. These results were soon published in the Journal of Dermatologic Surgery and Oncology in 1990 and presented at the annual meeting of the American Society for Dermatologic Surgery in March 1991.
These initial works inspired many dermatologic surgeons to use botulinum A exotoxin (Botox® , Dysport®) for the treatment of the glabella (frown lines), crow’s feet, and forehead which was soon followed by other specialties including plastic surgery and ophthalmology. The addition of the carbon dioxide laser to the cosmetic surgeon’s armamentarium has resulted in a resurgence in the cosmetic surgery field. Dr. David Duffy in one of the pioneers who began using botulinum toxin with laser resurfacing which was reported by the Carruthers in Dermatologic Surgery in 1998. Soon thereafter, trials were begun using botulinum A exotoxin in combination with other cosmetic procedures including endoscopic brow lift, upper and lower blepharoplasty (eyelid surgery), and in the lower face with facelifting. Platysmal bands, which are found in the front of the neck, were found to be responsive to treatment with botulinum A exotoxin by Blitzer et al. The treatment of axillary hyperhidrosis (excessive sweating under the arms) and palmar hyperhidrosis (excessive sweating of the hands) was introduced in 1995 by Bushara et al. with moderate success.
Now, more than twenty-five years after Dr. Alan Scott first described the clinical use of botulinum A exotoxin (Botox®) for the treatment of strabismus (crossed-eyes), the clinical possibilities for botulinum A exotoxin is most limited by our imagination.
How long does the treatment take?
Most treatments can be accomplished within 10-15 minutes–one of the so-called “lunch-time” procedures. Most patients will have no evidence of having anything done, although some will have mild bruising (particularly when treating the Crow’s feet).
Do I need to take off from work or other activities?
For 3-4 hours after the procedure it is recommended that the patient remain in the upright position. Additionally, it is best to avoid strenuous or jarring activities such as exercising, running, or jogging for at least 3-4 hours. Nearly all patients may return to work immediately following the procedure and resume exercise the following day?
Do the treatments hurt?
The treatments consist of a series of tiny injections using a fine needle. Although most patients tolerate the treatments with little discomfort, some patients request the use of a topical anesthetic which is applied to the areas to be treated 1-2 hours before the scheduled appointment.
How much does Botox® treatments cost?
The toxin itself is expensive. The cost varies from doctor to doctor, and depends on which area(s) are to be treated. Some doctors charge according to the amount of toxin used while others charge per “zone” treated. The average cost per “zone” is approximately $260.00 – $500.00. A “zone” would be any one of the following: glabella (frown lines), forehead, or crow’s feet.
What is Botox® ?
Botox® is a toxin (toxic substance) which is naturally produced by the bacteria called Clostridium botulinum. Interestingly, it is currently believed to be the most toxic poison known to man, although the use of such tiny amounts has been used safely in man for over twenty-five years. This bacteria produces several types of toxin, of which only “type A” is used for medicinal purposes today.
How does Botox® work?
The Botox® toxin works where the nerve meets the muscle where the nerve sends its signal telling the muscle to contract. This results in paralysis of the treated muscle.
How long does a Botox® treatment result last?
Unfortunately, Botox® results are not permanent. Initial treatments for wrinkles typically last 3 to 4 months. Subsequent treatments may prove to have more lasting results. Treatment of hyperhidrosis (excessive sweating) may last up to one year (average 5.2 months)
What wrinkles can be treated using Botox® ?
Although Botox® is only FDA approved for treatment of the frown lines (glabella), Botox® has been used with good to excellent results for the treatment of the forehead wrinkles and crow’s feet. Infraorbital wrinkles (wrinkles below the eyes) can be treated with moderate results. Newer therapeutic uses have been for the treatment of nasolabial folds (smile lines), perioral wrinkles (wrinkles around the mouth), corners of the mouth, and anterior neck which carry a higher risk of complications and have mixed results.
Can Botox®treat excessive sweating (hyperhidrosis)?
Yes. Botox® has been recently FDA approved to treat hyperhidrosis of the hands and axilla (underarms) since at least 1995 with good results which may last up to 12 months (average 5.2 months). Treatment of the hands has resulted in mild weakness of the hands in a few patients as a result of toxin diffusion to the intrinsic muscles of the hand (muscles within the hand). Since this finding, more superficial injections have been used with good success and a lower incidence of weakness.
Who should not get treated with Botox®?
Botox® has not been studied in pregnancy, and it is therefore unknown if fetal harm will result if a pregnant woman is treated with Botox®. Therefore, the use of Botox® is not recommended during pregnancy. Additionally, it is unknown if Botox® (botulinum A exotoxin) is excreted in breast milk, where it could affect a nursing infant. Therefore, Botox® treatment is not recommended for use in lactating women. Additionally, patients with neuromuscular disease, such as myasthenia gravis and Eaton-Lambert syndrome, should not be treated with Botox® as it may worsen these conditions. Of course, anyone who has had an allergic reaction to Botox® should not be treated.
What are the side effects and complications (problems) associated with treatments with Botox® ?
As Botox® is injected directly into the muscle body when used for wrinkles, bruising may occur. This can be minimized if patients avoid the use of aspirin, aspirin-containing products, and non-steroidal anti-inflammatory agents (i.e. ibuprofen, Motrin® , Advil® , naproxen, Aleve) for one week before treatment, although this is not necessary. Rarely, generalized reactions have been reported include nausea, fatigue, malaise, skin rash, and flu-like symptoms. It has been postulated that these generalized reactions occur from diffusion of minute amounts of the toxin into the circulatory system of which the significance of such reaction is unknown.
With treatment of the glabella (frown lines), ptosis (drooping of the eyelid) has occurred and may persist for up to 4 weeks. Some physicians believe that if patients remain in an upright position, avoid manipulation of the area treated, and actively contract the muscles treated for 4 hours after treatment, the likelihood of ptosis (drooping) is minimized due to increased uptake of the toxin. To avoid this problem, physicians are using more concentrated toxin that results in far less diffusion (spread) of the toxin to unwanted areas and therefore even less chance of eyelid droop (ptosis). In addition, most cosmetic surgeons believe that injections over the pupil should be at least 1 cm above the eyebrow. Although ptosis is now rarely seen, it is easily treated using alpha-adrenergic agonists (mild stimulants) topically applied to the eye (eyedrops).
Occasionally the glabella (frown lines) does not respond as well as one would like (i.e. frowning still occurs), especially in men. Therefore, this area may require a second treatment in 10-14 days.
Treatment of the forehead results in a more youthful appearance (due to decreased furrows), although there is decreased expressivity. Treatment must be carefully individualized to each patient. Patients who have a low brow and/or hooding of the upper eyelid (drooping upper eyelid skin) may have a total inability to raise any part of the eyebrow and may result in brow ptosis, worsening the appearance of the eyes. This can result in decreased visual acuity and the feeling of a ‘heavy brow’. Unfortunately, there is no treatment for this if it occurs, although the effects will wear off within 3-4 months. To avoid this, most cosmetic surgeons believe that treatment of the forehead should be above the first forehead wrinkle or at least 1-cm above the eyebrow. This may allow for some movement of the eyebrow. When the lateral fibers of the frontalis muscle (forehead muscles which wrinkle the forehead) have not been adequately paralyzed, a quizzical appearance may result in which one or both of the lateral eyebrows can be raised while the central portions remains depressed. This can be easily remedied by treating the lateral frontalis muscle (forehead muscles which wrinkle the forehead).
Bruising often follows treatment of the crow’s feet, occurs occasionally with treatment of the forehead, and rarely with treatment of the frown lines. Drooping of the lower lid margin and double vision have been reported, which can be avoided by injecting the toxin at least 1 cm from the lateral canthus (corner of the eye).
Treatment of the platysma (neck bands) has been reported to result in dysphagia (difficulty swallowing). Treatment with meloclopramide (Reglan) may improve swallowing if this occurs.
Treatment of the palms for hyperhidrosis (excessive sweating) has been reported to result in slight hand weakness in some patients. It is presumed that this has occurred due to diffusion of the toxin to the intrinsic muscles in the hand (muscles within the hand). Injecting the toxin very superficially has minimized this complication.
Therapeutic failures (patients do not respond to treatment) have now been reported. It is believed that these failures result when the body makes antibodies against the toxin, therefore neutralizing it. It is believed that with cumulative doses exceeding 200-300 Units, there is an increased likelihood of developing neutralizing antibodies. Therefore, when treating hyperhidrosis or larger muscle groups, it is recommended that injections be spaced at least 1-month apart. In the future, different types of this toxin may become available for clinical use that may be useful for those who have developed neutralizing antibodies.
Although Botox® is often used to treat migraine headaches, there have been a few reports of recurrent headaches occurring in patients undergoing treatment with Botox® for cosmetic purposes.
History of Botox® use:
In the early 1970’s, Dr. Alan Scott began investigating the use of botulinum A exotoxin for the treatment of strabismus (crossed-eyes) in monkeys. In 1977 clinical studies were initiated in humans for the treatment of strabismus. In the mid-1980’s Dr. Scott indicated that he had treated a patient for “cosmetic reasons” using botulinum A exotoxin.
Shortly thereafter, a patient of Dr. Jean Carruthers, an ophthalmologist in Vancouver, Canada, had noticed improvement of the glabella (frown lines) after a patient was treated for blepharospasm (twitching of the eye). This finding prompted Dr. Jean Carruthers, with Dr. Alastair Carruthers, a dermatologist also practicing in Vancouver, Canada, to begin the use of botulinum A exotoxin (Botox®) for the treatment of the glabella (frown lines) and, shortly thereafter, the treatment of the crow’s feet. These results were soon published in the Journal of Dermatologic Surgery and Oncology in 1990 and presented at the annual meeting of the American Society for Dermatologic Surgery in March 1991.
These initial works inspired many dermatologic surgeons to use botulinum A exotoxin (Botox® , Dysport®) for the treatment of the glabella (frown lines), crow’s feet, and forehead which was soon followed by other specialties including plastic surgery and ophthalmology. The addition of the carbon dioxide laser to the cosmetic surgeon’s armamentarium has resulted in a resurgence in the cosmetic surgery field. Dr. David Duffy in one of the pioneers who began using botulinum toxin with laser resurfacing which was reported by the Carruthers in Dermatologic Surgery in 1998. Soon thereafter, trials were begun using botulinum A exotoxin in combination with other cosmetic procedures including endoscopic brow lift, upper and lower blepharoplasty (eyelid surgery), and in the lower face with facelifting. Platysmal bands, which are found in the front of the neck, were found to be responsive to treatment with botulinum A exotoxin by Blitzer et al. The treatment of axillary hyperhidrosis (excessive sweating under the arms) and palmar hyperhidrosis (excessive sweating of the hands) was introduced in 1995 by Bushara et al. with moderate success.
Now, more than twenty-five years after Dr. Alan Scott first described the clinical use of botulinum A exotoxin (Botox®) for the treatment of strabismus (crossed-eyes), the clinical possibilities for botulinum A exotoxin is most limited by our imagination.
How long does the treatment take?
Most treatments can be accomplished within 10-15 minutes–one of the so-called “lunch-time” procedures. Most patients will have no evidence of having anything done, although some will have mild bruising (particularly when treating the Crow’s feet).
Do I need to take off from work or other activities?
For 3-4 hours after the procedure it is recommended that the patient remain in the upright position. Additionally, it is best to avoid strenuous or jarring activities such as exercising, running, or jogging for at least 3-4 hours. Nearly all patients may return to work immediately following the procedure and resume exercise the following day?
Do the treatments hurt?
The treatments consist of a series of tiny injections using a fine needle. Although most patients tolerate the treatments with little discomfort, some patients request the use of a topical anesthetic which is applied to the areas to be treated 1-2 hours before the scheduled appointment.
How much does Botox® treatments cost?
The toxin itself is expensive. The cost varies from doctor to doctor, and depends on which area(s) are to be treated. Some doctors charge according to the amount of toxin used while others charge per “zone” treated. The average cost per “zone” is approximately $260.00 – $500.00. A “zone” would be any one of the following: glabella (frown lines), forehead, or crow’s feet.