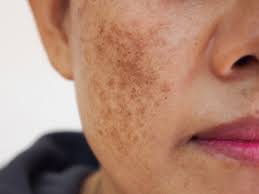
Melasma is a benign process in which brown spots appear on sun-exposed areas, most commonly on the face. Areas that are subject to the most sun are most frequently affected, including the forehead, upper lip, cheeks, and chin, although other areas can be affected.
Chloasma is melasma that occurs in someone that is pregnant.
What causes Melasma?
Genetics plays a key role in the development of melasma. Almost 48% of women report that another family member has the condition. The condition is also seen commonly in both identical twins. Ultraviolet light exposure plays a key role. Both UVB and UVA can increase the production of pigment in the skin. Hormones also plays a role in many patients. Estrogen, progesterone, and melanocyte-stimulating hormone (MSH) levels are normally increased during the third trimester of pregnancy leading to the increased production of pigment. Birth control pills containing estrogen can commonly lead to the worsening or development of melasma.
How can I prevent Melasma or maintain my complexion?
- Avoid sun exposure
- Use a SPF 45 or greater broad spectrum sunscreen that blocks both UVA and UVB. Here are a few good recommendations: SUNSCREENS. This measure alone will significantly reduce the risk of developing Melasma.
- Wear a wide-brimmed hat and sun-protective clothing when outside during the daytime.
- Avoid estrogen containing birth control pills
- Apply a stable topical Vitamin C product with Ferrulic acid daily that helps even out skin tones and prevent ultraviolet damage. Here is a recommendation: Cerum
How is Melasma treated?
All of the things that we recommend to prevent Melasma must be employed. Strict sun-avoidance is paramount. The use of a broad spectrum sunscreen daily is required as any sun-exposure, even for minutes, will stimulate the melanocytes to make more pigment. The use of sun-protective clothing, especially a wide-brimmed hat, is recommended if sun-exposure will be prolonged. One should avoid taking any estrogen-containing products (i.e. many birth control pills). Treatment can be very difficult and frustrating.
Hydroquinone: Topically applied hydroquinone can help lighten the skin by reducing the production of melanin from the melanocytes. Over-the-counter preparations containing 2% hydroquinone are available, but often are not effective enough. Here is an example of a good OTC bleaching cream: Fade 1 2 3 . These creams should be applied twice daily and only to the dark areas, as it will bleach any skin that it is applied to. Often prescription strength 4% hydroquinone is used, but results are often disappointing. Prescription compounds that contain higher concentrations of 7- or 8-% are commonly used and combined with other chemicals that often have very good results. These compounds are formulated by a compounding pharmacy and require a prescription.
Retinol, tretinoin, and other Vitamin A derivatives: Combining hydroquinone with a Vitamin A derivative, such as Retinol or tretinoin, is very helpful. Here is an example of a potent retinol that is available without a prescription: Tretinol. Retinols should be used at night and can be irritating. One should only apply a tiny pea-sized amount to the entire face and start slowly, maybe twice a week. If tolerated, one can even go up to twice a day if no irritation occurs. Tretinoin (Retin-A) requires a prescription and is often compounded with hydroquinone and other chemicals to produce the best results.
Topical Vitamin C: Oral Vitamin C is not helpful in preventing or treating Melasma. Topically applied Vitamin C is helpful in both preventing darkening of the skin and for the treatment of Melasma. For the treatment of Melasma, Vitamin C is often added to prescription creams (i.e. hydroquionone and tretinoin. Stand-alone topical Vitamin C is readily available without a prescription and can be used, although not all work the same. Most products are not stable, they oxidize, turn dark, and are not effective. This is a great product that has been shown to be helpful in both the treatment of Melasma and maintenance of results when combined with a sunscreen: Cerum
Laser and/or Chemical Peels: While some recommend these procedures, most treatments only help one third or patients and one third actually get worse. Therefore, one must exercise extreme caution when considering these procedures as the odds of having no improvement or worsening is greater then the chances of seeing improvement with most of these lasers and peels. When improvement is seen, it is not necessarily permanent and all other measures to prevent Melasma must be used or it will recur. Carbon Dioxide, Nd:Yag, Q-switched, and non-ablative lasers have all been used with mixed results and risk of worsening the condition. The 1540 Icon non-ablative laser has shown improvement ranging from 50-100% after only 3 treatments, but most patients will have a recurrence after treatment. Picosecond lasers and "Clear and Brilliant" have been used, have a lower risk of worsening the condition, and may be considered in moderate to severe cases. Superficial chemical peels may be considered and include Jessner's peel, Glycolic acid peel, and retinoic acid. More aggressive peels, such as tri-chloroacetic acid (TCA) should be used with extreme caution or avoided due to the risk of hyperpigmenation.
IPL (Intense Pulsed Light): This treatment is commonly used to treat darkening of the skin, but is it best for melasma? For mild to moderate melasma, the answer is maybe. In many cases, the condition improves after treatment only to worsen with time. For this reason, one must be extremely cautious and, for this reason, topical treatment is often preferred. For moderate to severe melasma, IPL can be considered and has been shown to be much more effective when combined with topical treatment. In general, IPL should only be considered in lighter skin types, if at all.
Dr. Bader's thoughts on lasers and IPL for Melasma: It is Dr. Bader's opinion that it is always best to start with a strong bleaching cream that is compounded, avoid exposure to Sun, and use a high SPF sunscreen with at least 12% physical blockers (zinc oxide and/or titanium dioxide). If one does not have the desired results after at least 10 weeks of treatment with faithful Sun avoidance and use of sunscreen daily, other treatments can be considered including picosecond lasers, IPL, and Icon 1540 non-ablative laser. Unfortunately, recurrence is common and patients should EXPECT this.
