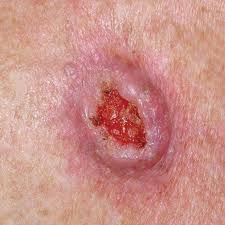
Squamous Cell Carcinoma
Squamous Cell Carcinoma is the second most common type of skin cancer that is most commonly caused by ultraviolet radiation that results from many years worth of sun exposure. For this reason, this type of tumor most commonly affects sun-exposed skin, such as the face, arms, and lower legs. Less commonly, arsenic ingestion, some wart viruses (human papilloma virus), chronic skin ulcerations, and radiation exposure may cause squamous cell carcinoma.
Tumors may be invasive or may only be in the top layer of skin (in situ).
Invasive Squamous Cell Carcinoma
When the tumor cells are found in the dermis of the skin or deeper layers, it is said to be an invasive tumor. When tumor cells are present in these deeper layers of the skin, they can spread through the bloodstream to the lymph nodes or other organs--"metastasize". In general, the risk of metastasis is very low and estimated to be approximately 3% of all squamous cell carcinomas. Tumors that occur within a burn scar and those that are on the lip or ear are more likely to metastasize than those elsewhere and carry a risk of up to 15%. There are other factors that increase the likelihood of metastasis, which include: very large size, poorly differentiated tumors on pathology, and the genetic make-up of the tumor cells that can be tested to assess metastatic risk.
Evaluation of Squamous Cell Carcinoma
Invasive tumors with one or more high-risk features, may be genetically evaluated to determine risk of metastasis. High risk factors include: tumor greater than 2cm, tumors located on the head, neck, hands, genitals, feet or front of the leg, immunosuppression, history of prior and history radiation at the site of the tumor. This test may be the most accurate in determining the risk of metastasis and only involves testing on the original biopsy specimen. Go to www.castletestinfo.com for more information.
Treatment
In most cases, surgery (Mohs' micrographic surgery, excision, or electrodessication and curettage) or radiation is used to treat these invasive tumors. There are pros and cons to each treatment method with differences in cure rate, healing time, post-treatment restrictions, and cosmetic outcome.
Squamous Cell Carcinoma in situ (Bowen's disease or intraepitheelial squamous cell carcinoma)
Early, non-invasive tumors are called squamous cell carcinoma in-situ (or intraepithelial squamous cell carcinoma or Bowen’s disease when caused by the Sun), which does not pose a metastasis risk at this early stage. In situ means that the tumor cells are only present in the epidermis, the top layer of skin, where there are no blood vessels and therefore there is virtually no risk of spreading. This early variant is not life-threatening unless untreated, in which case it can become invasive with time (months to years).
Treatment
Both non-surgical (i.e. imiquimod cream, 5-FU) and surgical (Mohs' micrographic surgery, excision, or electrodessication and curettage) treatment options exist for this early form of cancer.
Keratoacanthoma or Squamous Cell Carcinoma, Keratoacanthoma Type
There is much confusion over this tumor in recent years. This tumor was considered to be a "benign" or "pre-malignant" tumor for decades. These tumors typically grow very rapidly for several months, the stop growing, and then spontaneously involute (go away leaving a scar). More recently, reports arose of "metastatic keratoacanthomas"--tumors that did in fact metastasize (spread). It is still questionable whether or not these "metastatic lesions" were in fact keratoacanthomas or a squamous cell carcinoma. Unfortunately, it is sometimes difficult to know for sure. For this reason, nearly all textbooks are advocating removal of these lesions despite the incredibly rare risk of this occurring. This has resulting in numerous procedures that, in all likelihood, are unnecessary. Hopefully, in the upcoming years this will become clearer and a true distinction can be made between keratoacanthoma and squamous cell carcinoma.
Treatment
While surgical removal is currently recommended for most, the choice to clinically observe the lesions is viable and is a great option for many. In my experience, over 95% of these lesions resolve after biopsy within 6-8 weeks. When lesions exhibit aggressive behavior, fail to involute, or increase in size, consideration should be given for complete surgical removal.