Skin Cancer Detection | Skin Cancer Treatment Skin Cancer Screening
Good versus Bad Dermatologist
A "competent" Dermatologist looks at a lesion and is fairly certain that it is cancer or not.
A good and honest Dermatologist takes a biopsy of a "suspicious" lesion and 50% or more of the time it proves to be cancer.
Sometimes patients will state that they "don't like their dermatologist because he or she always take biopsies". If a Dermatologist takes biopsies and they prove to be cancerous, he or she is doing a good job! On the other hand, if he or she takes biopsies and they always seem to be benign, it may be time to find a new Dermatologist!
A "bad" or dishonest Dermatologist takes biopsies that nearly always proves to be benign. This is not a "thorough" Dermatologist. This is a bad or dishonest Dermatologist as these biopsies are unnecessary. This is someone that I would not want to be my Dermatologist.
If you are searching for "an honest and reliable skin cancer detection center near me', RSB Dermatology is here to help.
Skin Cancer Screenings & Why You Should Get It
It is well known that skin cancer screenings should be a part of most peoples general care. Most cancers that are treated in my office (approximately 70%) are found during these screenings--not during routine physical examinations, not by patients, not by any other physician.
These screenings are a VISUAL inspection. It is recommended that one get completely undressed and examined from head to toe. There is no substitute for this type of screening.
If you are looking for a 'skin cancer screening near me', RSB Dermatology is here to help!
How is Skin Cancer Treated
There are both surgical and non-surgical treatment options available for many types of skin cancer.
CLICK HERE TO READ ABOUT THE DIFFERENT TREATMENTS FOR SKIN CANCER
A decision on which treatment to choose is a patient's decision. Dr. Bader will discuss the options with you and will be based on several factors, which are listed below.
Based on those 5 factors, a patient can make a choice on what is best for him/her depending upon their own priorities. There is no single treatment that is best for every person, every tumor, or every situation. Treatment must be personalized for each individual.
If you are looking for an 'honest and reliable opinion or skin cancer treatment near me', RSB Dermatology is here to help.
As far as surgical cure, Mohs' Micrographic Surgery has the lowest recurrence rate of any treatment for the treatment of basal cell carcinoma, squamous cell carcinoma, melanoma in situ, dermatofibroma sarcoma protuberans, atypical fibrohistiocytoma, malignant fibrous histiocytoma, Merkel cell carcinoma, and some other tumors.
Radiation has the second lowest recurrence rate for basal cell and squamous cell carcinoma (as low as 3% for untreated cancers).
Surgical excision or Mohs' Surgery WITH reconstruction (not second intention) often have the fastest healing time.
Topical creams can look irritated for a few weeks. Radiation can result in "radiation dermatitis" that can look very irritated for a few weeks or longer.
Sutured wounds (from excision or Mohs' with reconstruction) usually require the least amount of after-care. Electrodesiccation and curettage requires once or twice daily wound care for 3 weeks to 3 months or even longer. Radiation may require some care in the event of acute radiation dermatitis that may occur. In some cases, skin ulceration occurs after radiation, for larger lesions or those on the lower extremities, that can take months to heal.
The topical creams are often the least expensive option ($16-28 + office visit charges), while radiation is often the most expensive ($4000 to over $30,000). Surgeries that are performed in a doctor's office are far less expensive than those performed in a surgery center, even when in a doctor's office, or hospital. If another doctor closes a wound after Mohs' surgery, the cost is usually twice as much as when the Mohs' surgeon closes the wound immediately after Mohs'.
Topical treatments (creams) usually have the best cosmetic outcome. Radiation can have a great outcome, but should be reserved for those whom are not surgical candidates or who are older. Mohs' surgery does not result in a "bad scar", it is the "reconstructive surgery" after the Mohs' that will determine how the wound will look to a large degree.
Skin cancer detection:
How is Skin Cancer Diagnosed?
The diagnosis of skin cancer is almost always done by a visual inspection. The Dermatologist will look at the suspicious lesion and make a determination whether or not it is likely or possibly malignant (cancerous). For some pigmented lesions, dermoscopy (a magnifying lens with a light at the periphery) can be used to assist in this decision making process.
If a skin cancer is suspected, a skin biopsy is taken, sent to a laboratory, and evaluated under the microscope by a Dermatopathologist--a doctor who specializes in skin pathology. In some cases, special tests are performed in the lab to look at specific proteins that may be present in the skin. The proteins tested for help differentiate between benign and malignant tumors or the type of tumor, thus helping the dermatopathologist come to an accurate diagnosis.
A diagnosis will be given based on that pathological examination of all tests under the microscope.
While there are some electronic or photographic devices, or even phone apps now, that can help "assist" with this process, there is nothing that is better than the well-trained naked eye of a board-certified Dermatologist and a Dermatoscope.
What is a skin cancer screening?
A screening is recommended for all patients. This should be performed by a board-certified Dermatologist, who is trained in detecting skin cancer. This is a visual inspection of the skin. The Dermatologist will not just look at a specific lesion, but all the skin--from head to toe.
How is a skin cancer screening performed?
People are commonly surprised when we ask them to disrobe for a skin cancer screening. A skin cancer screening is visual--the Dermatologist looks at the patient, preferably from head to toe, and even between the toes. Many patients assume that patients are screened like they do in an airport--fully dressed and scanned by a machine. This is not the case! The doctor must see the skin. Photographs may be taken. Some will use computerized systems to evaluate the photographs, often done before the visit, which often looks for "new lesions" or "changes" in existing lesions.
Why is a skin cancer screening so important?
Most skin cancers are diagnosed during a skin cancer screening. They are NOT diagnosed by patients, their Primary Care Physicians, or their Plastic Surgeons. Therefore, a skin cancer screening should be a routine part one one's healthcare. For some types of skin cancer, early detection is critical to having a good outcome.
If you are in need of a 'skin cancer screening near me', look no further.
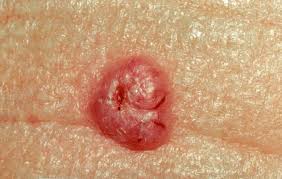
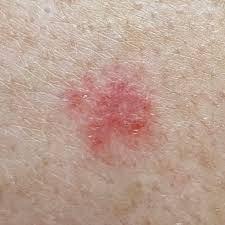
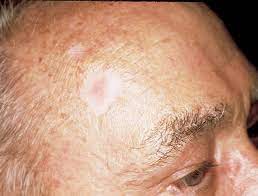
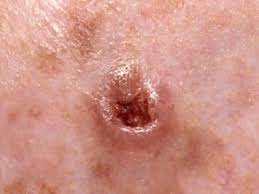
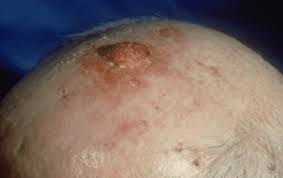
Basal Cell Carcinoma
This is the most common skin cancer and is rarely life threatening. If left untreated for many, many years it can be a serious problem. There are several different subtypes of basal cell carcinoma that are based on characteristics seen under the microscope (pathology).
Both surgical and non-surgical treatment options exist. One must take into account the location of the tumor, the histological subtype, and the size of the tumor when considering different treatment options.
CLICK HERE TO READ MORE ABOUT BASAL CELL CARCINOMA
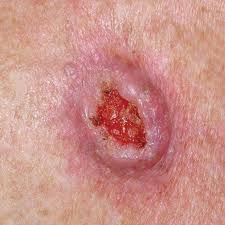
Squamous Cell Carcinoma
This tumor is caused by the sun when it occurs on sun-exposed skin. On other areas, such as the groin or around the nails, human papillomavirus (HPV), the virus that causes warts, is often the cause.
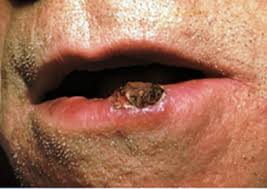
This tumor may be non-invasive (squamous cell carcinoma in situ, intraepithelial squamous cell carcinoma, intraepithelial squamous cell carcinoma) at which stage it does not spread. Invasive tumors (superficial squamous cell carcinoma, invasive squamous cell carcinoma) have the capacity to spread to the lymph nodes and other organs. In general, the risk of spread is approximately 3%, except when tumors appear on the lip or ear. Tumors on the lip or ear have a significantly higher risk of spreading to the lymph nodes (up to 15%). and prompt and complete removal is recommended.
Both surgical and non-surgical treatments exist. Treatment options will vary based on whether the tumor is invasive or not, the location of the tumor, the size of the tumor, the depth of the tumor, the age of the patient, and the overall health of the patient.
CLICK HERE TO READ MORE ABOUT SQUAMOUS CELL CARCINOMA
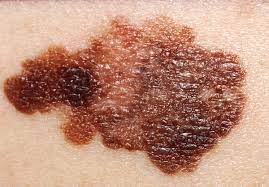
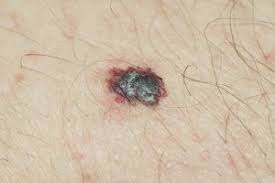
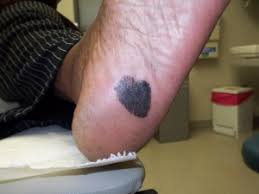
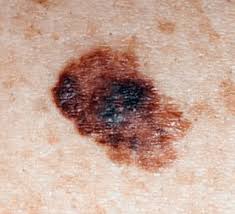
Malignant Melanoma
This is the third most common form of skin cancer. In most cases, these present as a irregularly shaped, pigmented lesion with irregular borders. Some types of melanoma may have no pigment and may be regular in shape. Many patients will report increasing size.
If a lesion is suspicious, Dr. Bader will take a biopsy and will discuss treatment options with you.
For all invasive melanomas, surgical treatment (excision or Mohs) is recommended. For non-invasive tumors (lentigo maligna or melanoma in situ), surgical removal (excision or Mohs) is the treatment of choice, although elderly or patients whom are not surgical candidates may consider imiquimod topical cream.